

Have questions about First Steps Recovery? We're here to help.
© Copyright 2023 • First Steps Recovery • All Rights Reserved
Depression is one of the most common mental health disorders experienced by individuals today. Unfortunately, many of those who suffer from depression turn to drugs or alcohol in an attempt to relieve themselves of the negative thoughts and feelings that depression causes. While some of these substances can alter a person’s state of mind, they’ll still feel the effects of their depression after the effects wear off. The person may continue to regularly abuse drugs or alcohol in order to alleviate the symptoms, becoming addicted in the process.
Addiction can actually increase symptoms of depression, whether through chemical imbalance or by cutting off systems of support. Entering into dual diagnosis treatment is the best option for an addicted person — they can learn how to address their depression without substances and address their addiction while taking their depression into account..


Depression is one of the most common mental health disorders experienced by individuals today. Unfortunately, many of those who suffer from depression turn to drugs or alcohol in an attempt to relieve themselves of the negative thoughts and feelings that depression causes. While some of these substances may alter the mindset of the individual consuming them for a time, after the effects of the substance wear off, the individual will still feel the symptoms of their depression. After symptoms of depression return, individuals may continue to regularly abuse drugs or alcohol in order to alleviate these symptoms, often resulting in instances of addiction. Over time, drug or alcohol addiction can actually increase symptoms of depression, which can be detrimental. Entering into dual-diagnosis treatment is the best option an addicted person has to treat both their drug or alcohol dependence as well as their co-occurring mental health disorder.
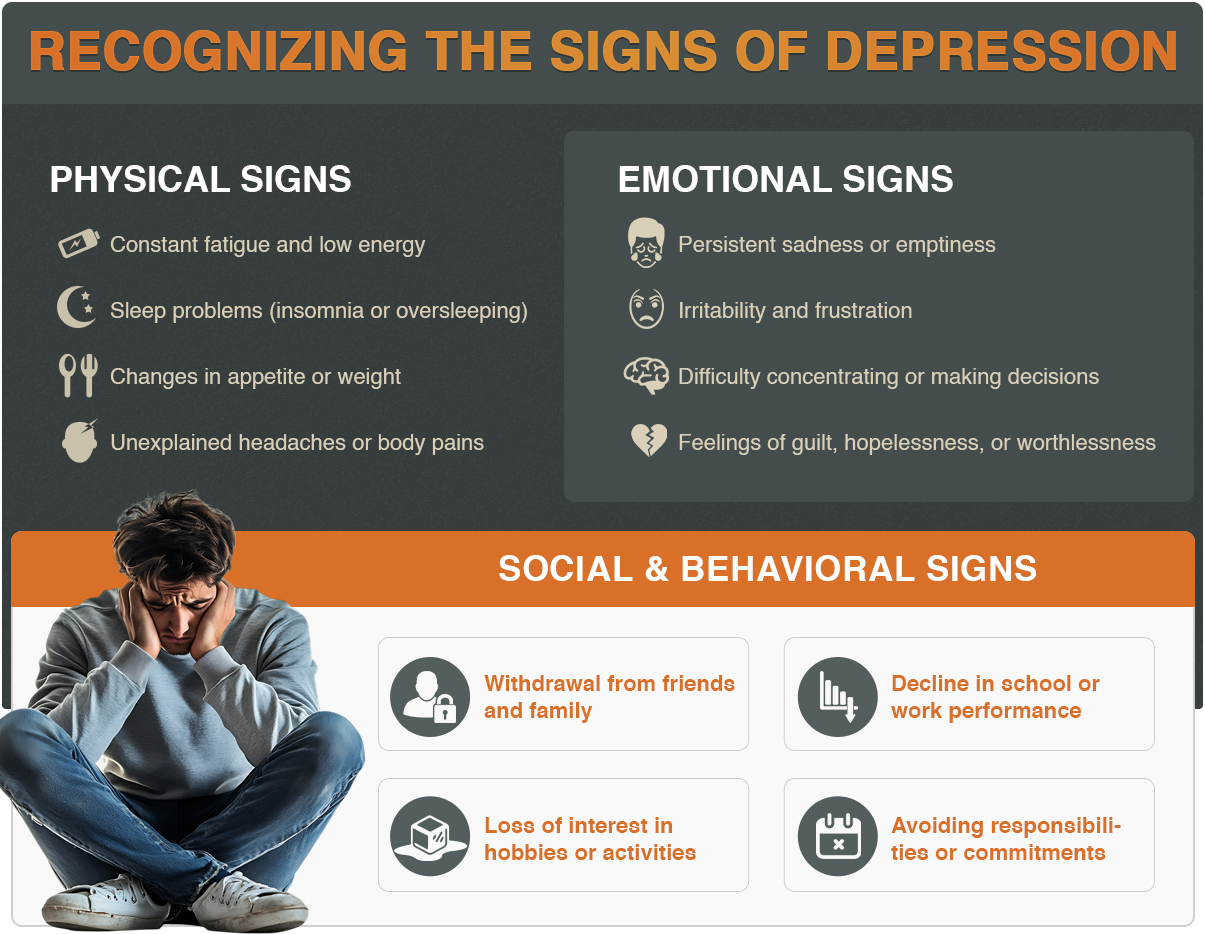

Depression is a complex mental health condition that can manifest in various ways, impacting individuals of all ages and backgrounds. It goes beyond just feeling sad or down; it can be a debilitating condition that affects a person’s overall well-being. Depression can cause issues when it comes to decision-making, as well as difficulty concentrating or thinking. Symptoms of depression are experienced over weeks or months and can worsen over time, leading to suicidal thoughts or ideations.
Furthermore, depression can also lead to irritability and anger outbursts, even over seemingly minor issues. This change in behavior can strain relationships and make it challenging for individuals to express their emotions effectively.
Mental health and physical health are intricately connected, and emotional distress can manifest as physical discomfort. These can be different from person to person. One person may have excessive sleep, while another may experience insomnia. What matters most is keeping track of symptoms and staying in contact with health professionals so treatment can be adjusted if needed.
Physical symptoms of depression may include:
Additionally, individuals battling depression may find themselves more susceptible to frequent colds or infections due to a weakened immune system. The body’s response to stress and prolonged feelings of sadness can compromise the immune system, making it harder to fight off illnesses.
Individuals struggling with depression may also experience intense feelings of guilt or worthlessness, often accompanied by self-critical thoughts and a distorted sense of self-esteem. The weight of these emotions can further contribute to the overall emotional burden carried by those grappling with depression.
Individuals with depression may find themselves caught in a cycle of thought, where their minds are consumed by repetitive and distressing thoughts. This can exacerbate feelings of sadness and hopelessness, which creates a feedback loop that reinforces the emotional symptoms of depression. Individuals may struggle to break free from this pattern, which can further deepen their emotional distress and sense of isolation.
Individuals experiencing depression may find it challenging to express their emotions and communicate effectively with other people. This difficulty in articulating their feelings can lead to misunderstandings in their relationships, causing further strain on their social interactions. But this may create barriers to seeking help and support, which may perpetuate a cycle of isolation and deepening depression.
The stigma surrounding mental health issues, including depression, can contribute to the social signs of this condition. People may fear judgment or rejection from others if they disclose symptoms of depression, which can lead them to hide symptoms and suffer in silence. This fear of being stigmatized can prevent individuals from seeking necessary treatment, as well as deepen their sense of social alienation.


Depression is a clinical diagnosis that is made by mental health professionals. To accurately diagnose depression, a healthcare provider will conduct a thorough evaluation, including a review of symptoms, medical history, and a physical examination. They may also order laboratory tests to rule out any underlying medical conditions that could be contributing to the depressive symptoms.
During the evaluation process, the healthcare provider will typically ask the individual about:
It is important for the individual to provide honest and detailed information to help the healthcare provider make an accurate diagnosis and develop an appropriate treatment plan. The professional needs to be able to assess the impact of depression on daily functioning, and the presence of any co-occurring mental health conditions (such as general anxiety).
There are various types of depression disorders, each with its own distinct characteristics. This is a small sample of the types of depression people may experience throughout their lives:
This is one of the most common forms of depression, characterized by persistent feelings of sadness or a loss of interest in activities. This can be caused by an event or not due to a single trigger.
Also known as persistent depressive disorder, this form of chronic depression lasts for at least two years. Symptoms can range from mild to severe. About 2.5% of American adults experience dysthymia at least once during their lifetime.
This form of depression occurs after childbirth, and may persist for some time after the child is born. Women can be diagnosed with this condition if they have feelings of depression, feelings like they don’t love their child, or feelings of being overwhelmed for two to four weeks after giving birth. It’s also been discovered that up to ten percent of new fathers may also experience postpartum depression, and that it may develop over time within a year of the child being born.
This form of depression occurs after childbirth, and may persist for some time after the child is born. Women can be diagnosed with this condition if they have feelings of depression, feelings like they don’t love their child, or feelings of being overwhelmed for two to four weeks after giving birth. It’s also been discovered that up to ten percent of new fathers may also experience postpartum depression, and that it may develop over time within a year of the child being born.


Addiction treatment centers, like the one here at First Steps Recovery, are staffed by knowledgeable and experienced therapists and medical professionals dedicated to helping clients correctly address their mental health conditions and overcome substance abuse disorder at the same time through our residential inpatient treatment program California.
Dual diagnosis treatment addresses both the addiction and the depression at hand, keeping in mind all the ways one may affect the other. This integrated method acknowledges the possibility that people may self-medicate themselves for depression using substances.
One key aspect of dual diagnosis treatment is the importance of personalized care plans. Each individual’s journey through dual diagnosis is unique, and therefore, treatment must be tailored to their specific needs. This may involve a combination of therapy, medication, support groups, and lifestyle changes to address both the mental health and substance abuse aspects of their condition.
The first steps of therapy always include a period of medical detoxification to fully purge the person of the addictive substances. It’s important to ensure that someone with depression has support during this time, because the intense symptoms may trigger a relapse in order to alleviate discomfort. Depression may also be aggravated at this time.
The key to understanding how addiction interacts with an existing mental disorder is working through it with a medical professional with expertise.Both individual and group therapy help individuals learn skills to help cope with their mental illness (and addiction!) without relying on substances. Specialty therapies like cognitive behavioral therapy (CBT) can help give people practical skills for dealing with depressive thoughts and working through temptations to use their addictive substances.
The symptoms of withdrawal can prove distracting or even debilitating when undergoing treatment for addiction. Treatment centers like First Steps can prescribe medications like methadone to help ease withdrawal symptoms so that individuals can focus on their recovery. It can also help determine the exact nature of a person’s depression without the distraction of substances.
Transitioning from treatment to the “real world” can be extremely stressful. It’s important to have continued support to maintain sobriety during that crucial time, whether it’s through support groups or an alumni program. People with a dual diagnosis of depression and addiction may wish to secure a therapist they can work with after they exit rehab.


From our certified therapists and nurses to our emotional support animal "Cooper", our entire team is dedicated to the health and success of our clients throughout our program and beyond.
Have questions about how our treatment programs works? Let's talk.
ADHD, or ADD, is a common neurodevelopmental disorder with attention and impulse control difficulties that can lead to substance abuse. Treatment with therapy and medication is crucial.
Anxiety disorder is a mental health condition characterized by excessive and persistent feelings of fear, worry, and apprehension that can significantly impact a person's daily life.
Bipolar disorder is a mental health condition characterized by extreme mood swings, including episodes of mania (elevated mood and energy) and depression (low mood and loss of interest).
Depression is a mental health disorder characterized by persistent sadness, loss of interest, and other emotional and physical symptoms
An eating disorder is a mental health condition characterized by abnormal eating habits. Getting help is important to address physical and psychological health risks, improve quality of life, and promote recovery.
Personality disorder is a mental health condition characterized by unhealthy patterns of thinking, behaving, and relating to others. Getting help is crucial to improve relationships, coping skills, and overall well-being.
PTSD (Post-Traumatic Stress Disorder)/Trauma disorder is a mental healtah condition resulting from experiencing or witnessing traumatic events. Getting help is important to process trauma, reduce symptoms, and improve overall quality of life.
Schizophrenia is a mental health disorder characterized by hallucinations, delusions, and disorganized thinking. Getting help is vital to manage symptoms, improve functioning, and enhance overall quality of life.
Have questions about our substance abuse treatment programs? Let’s talk.
Dayatra L.
Melissa B.
Bruce G.
Have questions about how our alumni program works? Let's talk.




















Have questions about First Steps Recovery? We're here to help.
© Copyright 2023 • First Steps Recovery • All Rights Reserved